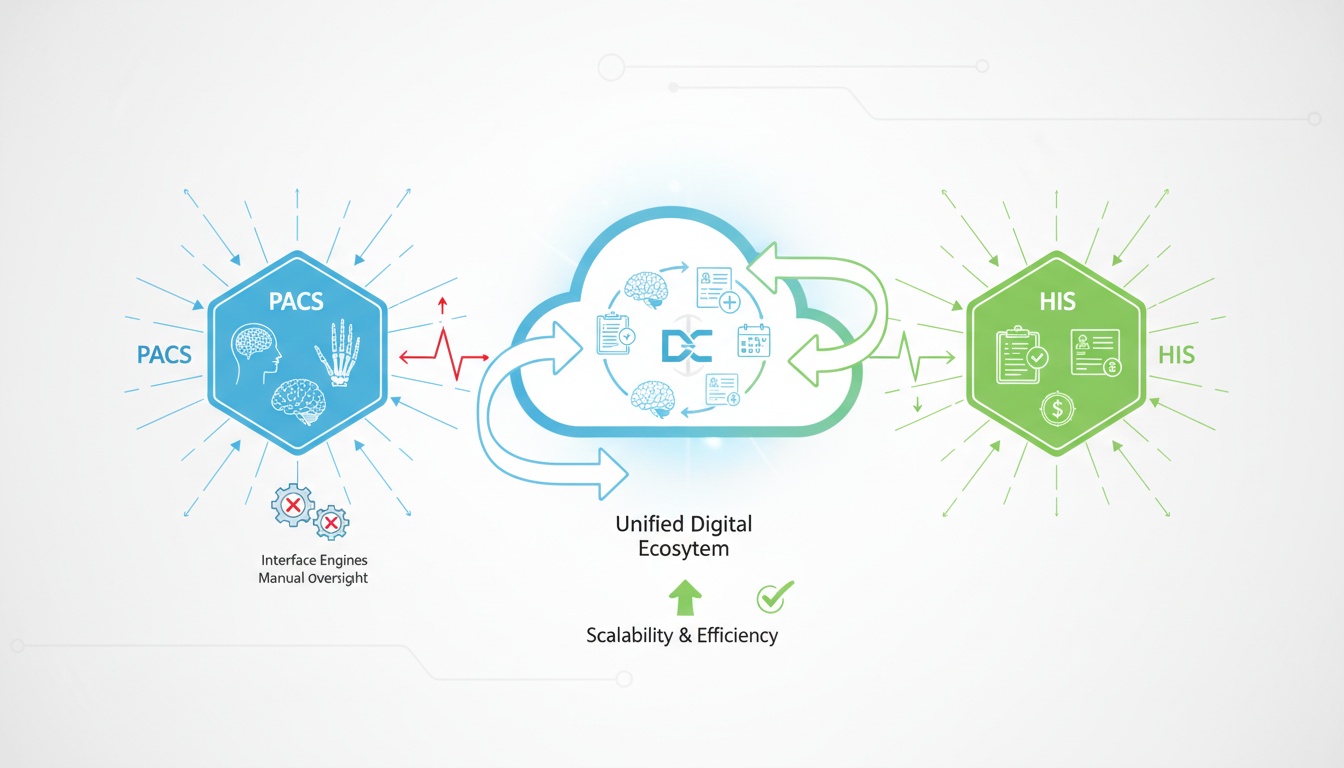
Modern healthcare systems are no longer based on silos in applications. Imaging data, patient demographics, diagnostic reports and administrative records need to operate in a unified digital ecosystem. Yet in the past, Picture Archiving and Communication Systems (PACS) and Hospital Information Systems (HIS) were often running parallel to each other instead of collaborating.
This separation resulted in inefficiencies of workflow, data reconciliation issues and technical dependencies that imposed a limitation on scalability. Radiology departments used PACS for image storage/retrieval, while hospital-wide systems kept track of patient records, admissions and billing processes. Bridging these systems had to be overseen by complex interface engines and required manual oversight.
As healthcare delivery expanded from single-site infrastructures, the problems of looser systems began to become more evident. Multi-site networks, remote reading environments, the expansion of telemedicine and data governance requirements called for greater integration between imaging and enterprise systems.
Today, integrated PACS with HIS is no longer a technical luxury -- it is a structural necessity. More importantly, cloud native architectures have fundamentally redefined the ways that interoperability is achieved, maintained and scaled.
Integrated PACS with HIS has evolved from the brittle interface-based connectivity to robust and cloud orchestrated interoperability.
• Early Integration Depended A Lot On Interface Engines Translating Hl7 And Dicom Standards.
• True Interoperability Requires Patient Identity Synchronization, Automated Worklists And Unified Report Workflows.
• Cloud Native Pacs Centralizes Integration Layers, Alleviating The Infrastructure Complexity Across Multi-site Networks.
• Security, Auditability And Compliance Need To Be Built In At The Architectural Level.
• Modern Integration Helps You Be Ready For Ai, Remote Collaboration And Scalable Enterprise Growth.
When designed strategically, integrated PACS and HIS systems move medical imaging from a departmental utility to a fundamental enterprise service.
With the modernizing of healthcare infrastructure that is taking place, the integration between imaging and hospital information platforms becomes fundamental rather than optional. Evaluating the connection of your PACS architecture with existing systems is a critical step toward scalable, resilient medical imaging operations.
Explore how the cloud PACS infrastructure of PostDICOM supports secure standards-based HIS integration across distributed healthcare environments.
Early PACS implementations were designed primarily as imaging repositories. The main thing they did was to turn images into digital pictures and get rid of the old way of using film. They wanted to use images instead of film for all their work, with radiological images. These systems were often deployed on-premise within radiology departments, optimized for high-volume image storage and diagnostic viewing rather than enterprise-wide data exchange.
At the same time, Hospital Information Systems evolved separately to manage administrative and clinical data such as admissions, discharge records, billing, and physician documentation. HIS systems were designed to work with text data not with high-resolution images.
The technical standards of the systems are what make them work the way they do for their purposes.
PACS relied on the DICOM standard to manage imaging data, while HIS platforms used HL7 messaging protocols to exchange patient and workflow information. Although both standards were essential to healthcare IT, they were not inherently interoperable. DICOM managed imaging objects; HL7 managed patient events and clinical orders.
To connect these systems, hospitals deployed interface engines or middleware brokers. These engines translated HL7 messages into worklist updates for PACS and ensured that patient identifiers were synchronized across platforms. While functional, these integrations were fragile. Changes in message structure, version mismatches, or network interruptions could disrupt workflows.
As hospital networks got bigger they needed more people to watch over the computer systems. Every time a new machine, department or building was added it made things more complicated, for the hospital networks. The hospital networks had to deal with this complexity.
Understanding integrated PACS with HIS needs knowledge of core standards. These standards help systems talk to each other. PACS and HIS must follow these rules to share information smoothly.
Health Level Seven or HL7 is a set of standards for sending messages, between healthcare systems. These standards help healthcare systems share administrative data with each other. When we talk about HL7 in the context of PACS integration there are types of messages that are really important:
• Adt (admission, Discharge, Transfer) Messages Update Patient Demographic And Status Information.
• Orm (order Message) Communicates Imaging Orders From His/ris To Pacs.
• Oru (observation Result) Transmits Finalized Reports Back To The Hospital System.
These messages help PACS match imaging workflows with hospital operations. If ADT is not synced patient identity mistakes could affect diagnosis accuracy.
DICOM governs the storage, transmission, and retrieval of medical imaging data. It tells us about file formats, metadata structures and communication protocols. These are used by imaging modalities and PACS systems.
When you do an imaging study, DICOM makes sure that the data from the machine can be saved, found, and gotten easily on systems. But DICOM does not take care of all the work that needs to be done in a hospital. That is why HL7 remains very important to hospital workflows. DICOM is good, for the imaging study data. Hl7 is needed to manage everything else that happens in the hospital.
As healthcare IT got more mature layers to help different systems work together came out to make things more flexible.
The DICOMweb system introduced a way to access images on the web using RESTful services. This is really helpful for people who work with images. The FHIR or Fast Healthcare Interoperability Resources made it easier to share information in a way using APIs. The DICOMweb and FHIR standards help us move away from systems and make it possible to integrate things in a more scalable way. This is good, for the DICOMweb and FHIR because they make things more flexible and easy to use.
In cloud-native environments, API-first architectures replace rigid point-to-point connections with service-based interoperability. he way we are building things now lets PACS-HIS integration work well in big healthcare networks that are spread out. This means PACS-HIS integration can get bigger without getting too complicated.
When PACS and HIS are two isolated systems, clinical workflows are based on synchronization and not integration. Radiologists may interpret studies contained in PACS, while patient demographics and clinical histories are contained within the hospital system. Any delay or mismatch between the two environments creates inefficiencies that are proportional to institutional size.
True integration makes a difference in the way these imaging workflows work on a daily basis across the enterprise.
When the ADT messages from the hospital system synchronizes in real-time with PACS, it immediately increases patient identity consistency. Imaging studies are automatically linked to accurate demographic information to minimize reconciliation errors and duplicate records. This isn't some minor administrative convenience - it has a direct impact on the safety of diagnostics and reliability of reporting.
Order communication is also streamlined. When an imaging request is placed within the HIS or RIS, an ORM message can automatically create a worklist entry within the PACS. Technologists no longer depend on manual data entry or systems of cross-referencing. The modality worklist is a dynamic list - this ensures that imaging studies are performed in the correct patient context.
Integrated environments also help in better report life cycle management. Once a radiologist completes a diagnostic interpretation, ORU messages can be used to return structured results back to the hospital system. Clinicians reviewing a patient's chart have access to imaging reports without having to go across multiple platforms. This united visibility helps to speed up treatment decisions and promotes better collaboration among disciplines.
In addition to radiology, enterprise integration allows cross-departmental access to imaging data. Imaging studies can be accessed by surgeons, oncologists, and emergency physicians via centralized frameworks for authentication. This cuts delays that are caused by departmental silos and enhances continuity of care.
In short, integrated PACS with HIS denotes a shift in the function of imaging from a department-centric to an enterprise-wide clinical asset.
While early models of integration used interface engines and localized middleware, in cloud-native architecture, there is a structural change in how PACS and HIS are communicating.
Traditional on-premise PACS deployments needed point-to-point integrations. Each hospital site had its own interface engine, its own hardware stack, and its own maintenance overhead. Scaling the environment required duplicating infrastructure from facility to facility, which provided increased cost as well as technical complexity.
Cloud PACS changes this model completely.
In a cloud native environment, PACS services run in elastic infrastructure. Integration is not dependent of static HL7 listeners or rigid interface brokers. Instead, modern systems use API-first design principles, microservices architecture, and event-driven communication layers.
This change has a number of structural benefits.
First, interoperability is centralized and becomes centralized, rather than distributed. A single integration layer for cloud can manage message processing, patient identity management, and authentication for several facilities. Instead of having disparate integrations for each site, healthcare networks can keep communication the same across locations.
Second, scalability is improved without corresponding proportional increases in infrastructure. As the volume of imaging increases, cloud-based systems dynamically assign computing and storage resources. Integration endpoints do not change even when throughput increases.
Third is that modern authentication frameworks provide additional security and traceability. OAuth2-based token systems, role-based access controls and encrypted data exchange replace old trust-based internal networks. This is particularly important in multi-site or remote access situations where VPN dependency previously created bottlenecks.
Cloud-native integration also provides for web-based imaging access via DICOMweb and via the use of a RESTful API. Clinicians are free to securely access imaging studies via browser-based viewers without having to install cumbersome client software. This enhances accessibility for remote radiologists, telehealth services and distributed care networks.
Importantly, it is cloud architecture which lessens single points of failure. Multi-region redundancy, which is the assurance that if one data center is disrupted, integration services will not be disrupted elsewhere. In mission-critical healthcare environments, this is not optional -- it is foundational.
By changing the integration approach between PACS and HIS from a local interface exercise to an infrastructure-level design strategy, cloud environments help redefine the role of imaging as a scalable, enterprise-ready service and not a departmental tool.
 - Created by PostDICOM.jpg)
Integration increases capability -- but it also increases responsibility.
When PACS and HIS are working independently, risk exposure is compartmentalized. Once systems become interoperable, patient demographics, imaging data, diagnostic reports and administrative workflows travel across interconnected environments. Without structured governance, this increased connectivity can increase vulnerability.
Modern integrated PACS-HIS environments must therefore include security at the architectural level instead of implementing it as an afterthought.
In integrated systems, user identification is critical, and user identity must be consistent. Radiologists, technologists, referring physicians, and administrative staff can use data on both the PACS and HIS platforms. Role-based access control (RBAC) frameworks make sure that users can only access information appropriate for their clinical or operational role.
Cloud-native environments enhance this model with centralised identity providers and token-based authentication mechanisms such as OAuth2. Instead of keeping credential silos for imaging and hospital systems, organizations can consolidate access governance across imaging and hospital systems. This is good for auditability as well as reducing credential sprawl.
Integrated systems continuously send and receive structured HL7 messages, imaging metadata data, and diagnostic content. All communication channels should be encrypted in transit using TLS protocols. Imaging archives stored in cloud infrastructure also need to implement encryption at rest, in order to prevent unauthorized data extraction even in the event of storage-level compromise.
Encryption is especially important for distributed healthcare networks where imaging may be accessed remotely across geographic boundaries.
Enterprise governance requires that you have complete traceability as to who accessed which records at what time. Integrated PACS-HIS environments need to record:
• User Authentication Events
• Study Access Activity
• Report Modifications
• Data Exports Or Downloads
Centralized audit logs help to tighten compliance oversight and make regulatory reporting easier. In multi-site networks of hospitals, centralized audit infrastructure also allows for cross-facility monitoring.
Healthcare organizations exist in a highly regulated environment, such as HIPAA in the United States and GDPR in the European Union. Integrated systems are required to assure:
• Data Minimization Principles
• Controlled Cross-border Data Transfer
• Documented Access Policies
• Breach Detection And Notification Protocols
Cloud-native PACS architectures tend to offer greater compliance tooling than legacy on-premise systems, such as automated monitoring, backup validation and structured retention policies.
Integration should not undermine compliance posture. On the contrary, if properly designed, it should reinforce transparency in governance between the imaging and administrative systems.
Beyond technical interoperability and regulatory alignment, integration will need to make sense in operational and financial terms.
Healthcare IT decisions demand more and more measurable results. Integrated PACS with HIS provides enterprise value by a number of dimensions.
Manual reconciliation between imaging systems and hospital records is time consuming and error prone. Automated synchronization helps reduce duplicate studies, minimize demographical inconsistencies, and easy order management. Over time, this enhances efficiency of staff and cuts the cost of rework.
Legacy environments often have several point-to-point integrations that they need to be monitored and updated constantly. Cloud-based integration layers centralize and standardize these interfaces and lessen the operational burden on IT departments.
Instead of having to keep separate middleware for each facility, healthcare networks can control integration from a unified architectural layer.
As hospital networks grow or acquire new facilities, the complexity of integration traditionally increases. Cloud-native PACS infrastructure enables new sites to connect via standardized API endpoints instead of duplicating entire hardware and interfaces stacks.
This has the side effect of dramatically shortening deployment times and lowering capital expenditure.
Unified worklists, synchronized patient data, and streamlined report return cycles mean turnaround times are reduced. Faster diagnostics reporting improves the patient flow and strengthens the overall patient care delivery efficiency.
Integrated cloud environments with multi-region redundancy provide better uptime guarantees. In disaster conditions, the imaging information and integration services are accessible. Business continuity planning is made infrastructure supported as opposed to manual.
When assessed holistically, integrated PACS-HIS environments transform from an IT cost centre to a performance enabler in terms of clinical, operational and financial domains.
Understanding modern integrated PACS-HIS environments requires an architectural shift visualization that has occurred in the last decade.
In legacy environments the integration often looked like this:
HIS → Interface Engine → PACS
RIS → Interface Engine → PACS
Modality → PACS
Viewer → PACS
All connections were point-to-point. Each site had its own infrastructure. Each update was at risk for interface disruption.
Cloud-native integration offers a more centralized and service-oriented architecture.
A modern integration model normally consists of:
• His/ris Sending Hl7 Messages (adt, Orm, Oru)
• A Cloud-based Integration Layer Processing And Validating Messages
• Identity Management Services For Synchronization Of Patient Context
• Cloud Pacs Storage And Image Orchestration
• Web-based Access For Viewing Via Dicomweb Apis
• Authentication Using Centralized Identity Provider
Instead of inflexible, location-specific pipelines, integration becomes a controlled service layer which can scale across facilities.
 - Created by PostDICOM.jpg)
Integration is no longer just the joining of two systems. It is about creating a flexible digital base that can support new healthcare technologies.
Several structural trends are influencing the next stage of PACS-HIS integration.
Healthcare software vendors are moving towards API-first. Rather than developing monolithic platforms, systems communicate with one another based on standardized service interfaces. This approach mitigates vendor lock-in and enhances the cross-platform interoperability.
Cloud-native PACS environments fit well with this model, allowing external applications -- such as analytics platforms and patient portals -- to access the imaging data in a secure manner.
Artificial intelligence tools are based on uniform and structured access to imaging data sets and corresponding metadata. When PACS and HIS exist in silos, AI implementation needs complicated data extraction pipelines.
Integrated architectures for the cloud make this process much easier. Imaging data studies and patient data can be accessed via secure APIs, speeding up validation and deployment of AI without having to rebuild infrastructure.
Telemedicine, remote reporting of radiology, and cross-border collaboration are becoming accepted parts of the care delivery. Integrated cloud PACS ensures imaging studies and reports are available no matter where the clinician is located.
This flexibility can be especially important for multi-site healthcare networks and international diagnostic partnerships.
Healthcare institutions are increasingly developing centralized data governance approaches. Integrated Imaging Infrastructure Contributes to Enterprise Data Lakes and Analytics Environments Rather than as isolated repositories of the image, PACS becomes a part of larger strategic data architecture.
The medical imaging storage, retrieval, and diagnostic viewing is managed by PACS (Picture Archiving and Communication System). HIS (Hospital Information System) handles patient information of administration, clinical, and patient records such as admission and billing, and physician documentation. Integration ensures that imaging workflows integrate with hospital-wide patient records and operational processes.
HL7 offers structured messaging standards so hospital systems can communicate patient demographics, imaging orders and diagnostic results. ADT messages are used to synchronize patient identity, while ORM messages are used to transmit imaging orders and ORU messages are used to return finalized reports. These types of messages enable PACS to exist within the larger hospital workflow ecosystem.
Yes. Modern cloud PACS platforms are based on API-first architecture and on standardized interoperability protocols (HL7, DICOMweb, FHIR etc.). This provides the ability to integrate with existing HIS, RIS, and EHR systems without the need for a full infrastructure replacement.
Properly designed integrated environments provide enhanced security from centralized identity management, data transmission encryption, audit logging, and role-based access controls. Cloud natively are often stronger governance frameworks than legacy on-premise integrations.
Multi-site healthcare organizations need a standard patient identity management with standard workflows and centralized governance. Integrated cloud PACS environments minimize infrastructure duplication and make imaging data available even across locations without impacting compliance or performance.
|
Cloud PACS and Online DICOM ViewerUpload DICOM images and clinical documents to PostDICOM servers. Store, view, collaborate, and share your medical imaging files. |