The last twenty years witnessed a radical shift in healthcare delivery, which was brought about by a digital transformation. Hospitals, clinics, imaging centers, and specialty practices now exist in even more complicated information ecosystems where large volumes of patient information are required to be documented, stored and shared among more than one clinical system. Based on lab outcomes and medication history, radiology reports, and treatment plans, the contemporary healthcare organizations rely on quality access to the information to come up with correct clinical decisions.
In the past, patient data used to be distributed in paper files, in records, of departments, and in isolated data systems. Such fragmentation frequently resulted in communication disconnects among providers, a sluggish process of diagnosis, and medical errors. The downsides of the previous record-keeping systems were becoming more pronounced as healthcare systems became larger and the number of patients increased.
Electronic Health Record (EHR) systems became a solution to these problems as they offer a centralized digitalized system that brings together patient data throughout the healthcare environment. EHR platforms integrated by consolidating clinical data into a single system allow physicians, nurses, specialists, and administrators to access the correct patient data in real-time. Such accessibility enhances coordination among departments greatly and facilitates quicker and better-informed clinical decision-making.
In addition to mere record digitization, the contemporary EHR systems are the backbone of connected healthcare systems. They are the core point upon which several clinical technologies engage, such as lab systems, pharmacy management platforms, medical billing systems, and diagnostic imaging systems like PACS. EHR systems can convert isolated healthcare technologies into data exchange with each other through standard interoperability frameworks such as HL7 and FHIR APIs.
With the further shift to integrated and data-driven care models in healthcare, the role of EHR systems has grown considerably. Clinical decision support tools, population health analytics, preventive care programs, and inter-institutional treatment planning are now supported on these platforms. The Electronic Health Record has, in a way become the digital heart of modern patient care management.
To respond to the question about the impact of EHR systems on healthcare quality, it is necessary to focus on how these systems change the clinical workflow of healthcare facilities, enhance the collaboration of the providers, and assist with making safer treatment decisions. The subsequent paragraphs explore five significant areas in which EHR technology is changing the quality of patient care, clinical collaboration, and healthcare data management in current digital health systems.
EHR systems have evolved to be the basics of the new healthcare infrastructure. Their impact reaches much further than mere digitizing of records and allows healthcare organizations to enhance the quality of care by managing it better and being more cooperative.
Some of the most important lessons of this article are the following significant changes brought about by EHR adoption in the current healthcare settings:
• Ehr Systems Regulate All The Patient Data And Enable Clinicians To Obtain The Complete Medical History Using One System.
• The Availability Of Real-time Data Enhances Clinical Decision-making, Especially In Situations Where There Is An Emergency Or Time-sensitive Treatment.
• Preventable Medical Errors Are Reduced Through The Use Of Automated Safety Measures, Including Allergy Alerts And Medication Interaction Warnings.
• Standard Workflows Streamline The Administration And Clinical Workflows, Enhancing The Efficiency Of Operations In Healthcare Organizations.
• Ehr Systems Have Population Health Analytics That Support Long-term Disease Management Programs And Preventive Care Strategies.
These capabilities can enable healthcare providers to provide more data-driven, patient-centered, and coordinated care.
Electronic Health Record (EHR) system is an online system which allows managing, storing, and sharing patient health information within healthcare institution(s). EHR systems present a wide and constantly updated picture of the medical records of a patient as opposed to traditional paper charts or departmental databases.
EHR systems are used to store a variety of clinical data, such as demographic data, physician orders, medication history, lab data, imaging order reports, treatment courses, and billing data. Such data is stored in a well-structured database that enables authorized medical personnel to access patient records in real-time at any clinical workstation connected to that database.
One of the assets of EHRs is their capacity to unify the information of various sources of the healthcare system. The interactions between a patient and a specialist can be automatically noted and coordinated as a patient undergoes diagnostic tests, takes medication, or communicates with specialists, and the patient has a digital record in which the interactions can be synchronized. This real-time data summarization forms a longitudinal and integrated perspective of the health record of the patient.
Electronic Medical Records (EMR) and Electronic Health Records (EHR) are terms that are interchangeably used when the two concepts are really different. EMR systems usually hold records of patients in a single healthcare institution, and they are mostly used as electronic substitutes for paper charts. EHR systems, in turn, are developed to provide interoperability and exchange data among the various healthcare providers and institutions.
This interoperability feature is especially essential in the contemporary healthcare conditions where patients frequently have to be treated by various experts and institutions. EHR systems can share patient data with external systems through standardized communication standards such as HL7 messaging and FHIR-based APIs, enabling healthcare networks to coordinate care.
Besides storage of clinical documents, most current EHR systems also have highly proficient features like clinical decision support systems, automatic safety warning systems, analytics dashboards, and features that allow patients to engage. Such capabilities enable healthcare organizations to record care and proactively enhance clinical outcomes with the help of data-driven insights.
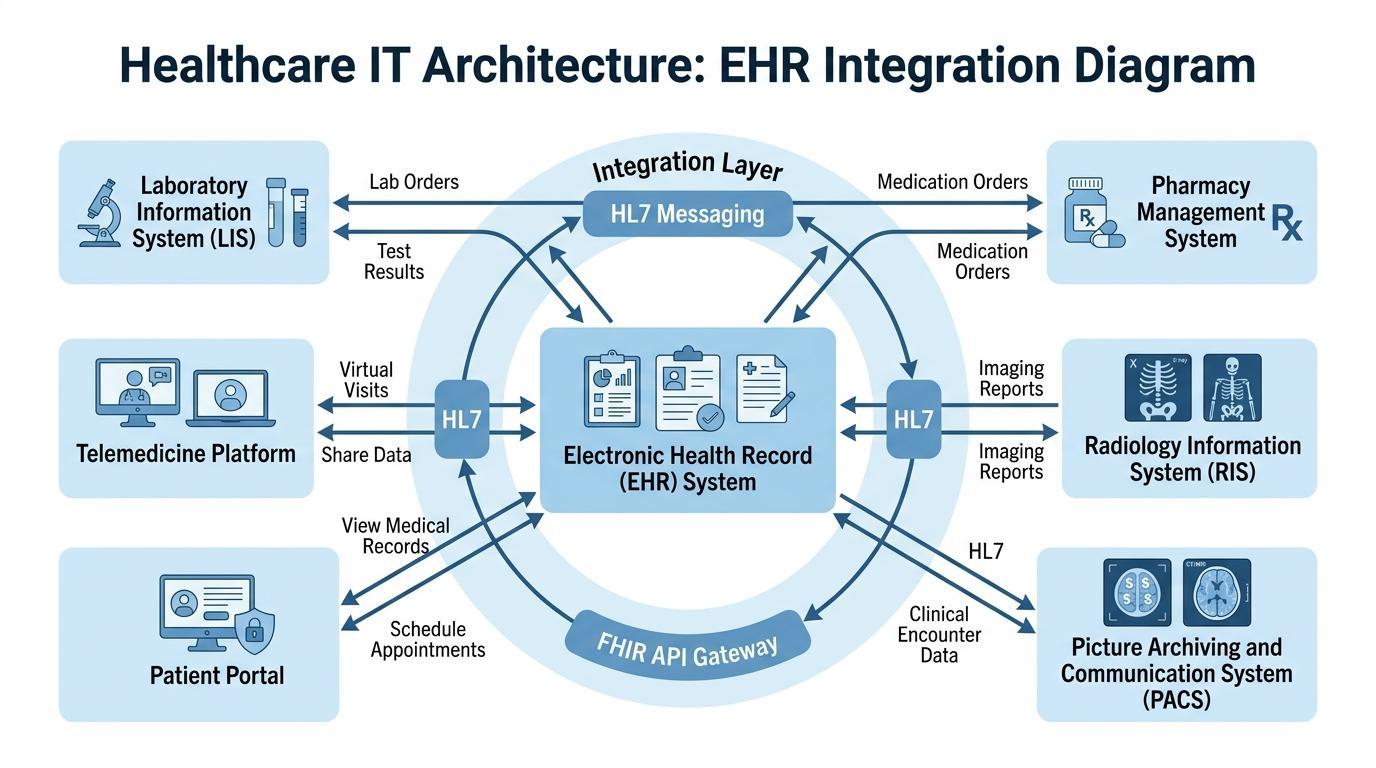
The necessity of the integrated digital infrastructure has never been as high as it is now because healthcare systems are growing and work with more specialized cases than before. Contemporary healthcare organizations are based on numerous clinical technologies which should interact with each other in an effective way to promote the process of effective diagnosis, treatment, and patient management.
The digitized healthcare ecosystem has its central coordination system in EHR systems. They integrate various operational and clinical technologies, and the healthcare professionals can access the necessary information without having to operate in different systems. Such integration enhances speed and accuracy of clinical decision-making.
A standard healthcare setting has EHR platforms communicating with a number of key information systems. The systems are Laboratory Information Systems (LIS) that handle diagnostic test findings, pharmacy systems that handle prescription of medicines, and the billing systems that handle administration and finances. Radiologic information systems and Picture Archiving and Communication Systems (PACS), as diagnostic imaging technologies, can produce significant amounts of imaging data which are also required to be available in the records of patients.
By connecting these systems, EHR platforms form a single environment in which patient information moves across departments in real time. A doctor who reads the chart of a patient will be able to get laboratory findings, imaging reports, medication history, and clinical notes without the need to change several software programs. Such a level of integration helps avoid considerable delays in diagnosis and enhances the coordination of care teams.
The emerging significance of interoperability standards has also empowered the purpose of EHR systems in healthcare infrastructure. Healthcare organizations can share patient information safely across institutions with the help of frameworks like HL7 messaging protocols and FHIR APIs to enable a wider collaboration between hospitals, clinics, and specialty providers.
Secondly, technologies of cloud computing and safe web-based platforms have allowed clinicians to gain access to patient records remotely. This feature justifies telemedicine projects, dispersed teams of healthcare professionals, and cross-institutional consultations, which are becoming more and more popular in contemporary healthcare delivery.
EHR systems are no longer perceived as documentation tools as healthcare continues to adopt the digital transformation. They rather serve as the core data exchange platform that facilitates integrated, coordinated, and patient-centered care throughout the healthcare ecosystem.
The systems of Electronic Health Records affect almost all the fields of contemporary clinical activity. These platforms are revolutionizing the process in which medical providers identify issues, organize care, and provide follow-up care through the centralization of patient data and real-time access to medical data.
EHRs are not digital repositories of medical records but do facilitate patient safety efforts and clinical workflows, as well as long-term healthcare planning. The five transformations discussed below demonstrate how the EHR technology has redefined the process of care delivery to patients in healthcare organizations.
Among the benefits of Electronic Health Record systems, the ability to access the patient's entire information quickly should be mentioned as one of the most important ones. Paper-based conditions were used when only a patient was required to find the medical history, and it may take a long time to find the files in different departments. Such delays may delay the process of diagnosis and treatment decision-making, especially during urgent care cases.
EHR systems remove these barriers since patient data is stored in centralized digital databases that can be accessed in real time by authorized health workers. Patient histories, lab results, imaging reports, medication records, and clinical notes can all be accessed through a single interface by physicians, nurses, and specialists. This holistic perception helps clinicians to see the totality of the health condition of a patient and then make decisions regarding their treatment.
Live access to data will be particularly important in the situation of an emergency when swift actions have to be taken. The emergency doctors have to work with patients who have complicated health histories and have to make decisions within a limited amount of time. Clinicians can have access to earlier diagnoses, allergies, medications, and previous treatments; with EHR access, they can check these items immediately and thus respond to clinical information more quickly and safely.
The other notable advantage of centralized patient data is the minimization of redundant testing. When diagnostic findings are readily available in the EHR, clinicians can review the laboratory reports and imaging studies to avoid ordering additional tests. This enhances efficiency, as well as minimizes unnecessary healthcare expenditures and the exposure of patients to repeat procedures.
EHR systems enable clinicians to make better-informed clinical decisions and directly improve patient outcomes by ensuring the availability of accurate, up-to-date medical information.
The process of healthcare delivery is becoming increasingly multidisciplinary, as it involves physicians, specialists, nurses, pharmacists, and allied health professionals. The coordination of care among such professionals is difficult without effective communication and access to shared patient information.
EHR systems support such collaboration by offering a platform that provides central access to review patient records, update care plans, and share clinical observations. Providers can communicate within the digital patient record in real time, rather than via telephone calls, fax transmissions, or manually transferred documentation.
This collective access to patient information enhances interdepartmental and interhealthcare facility continuity. As an example, a primary care doctor can make a referral and, at the same time, provide access to a medical history of the patient, laboratory test results, and medications, among others. This can be viewed by the specialist prior to the consultation, enabling him or her to conduct clinical assessments more effectively and efficiently.
The internal messaging and task management features of EHR systems can also help healthcare providers to better organize patient care. Doctors are able to send safe messages to colleagues, consultations can be requested, or instructions of care recorded in the patient record. Such communication tools minimize time loss and make sure that crucial clinical data are exchanged among the concerned care providers.
Collaboration can be enhanced, especially for patients who have complex or chronic conditions and thus need continuous care by various professionals. Treatment plans are more easily coordinated when every provider can access a shared patient record, and this is effective in avoiding conflicting therapies and achieving better long-term health outcomes.
Patient safety is among the most paramount concerns in healthcare provision, and EHR systems contribute a lot to minimizing the number of avoidable healthcare mistakes. In the pre-mechanized paper-based system, documentation would be handwritten, incomplete patient history, and minimal information exchange usually led to medication errors, misdiagnosis, and complication of treatments.
EHR systems overcome these vulnerabilities through the implementation of structured documentation, built-in safety checks, and built-in clinical decision support systems. These characteristics assist health care professionals in finding out suspected problems before they can impact the health of the patients.
Automated medication management is one of the most common safety provisions in EHR systems. The automaticity of the system enables physicians that prescribe medication via the EHR interface to verify the potential of drug interaction, allergies, or contraindications based on the medical history of the patient. In case of a conflict, the system will send an alert and make the physician review the prescription before making an order.
In the same manner, EHR systems will also be able to deliver clinical reminders and cautions about patient status, lab results, or treatment directives. As an example, a system could notify clinicians about abnormal test results that need to be followed up or about preventive screenings that are late. These computer checks are used to check that valuable clinical information is not lost in the hustly clinical routines.
Patient safety is also enhanced through the standardization of documents that are contained in EHR systems, which reduces ambiguity in clinical records. The use of structured templates and electronic data entry reduces the risks of illegible handwriting or missing chart entries. Consequently, healthcare providers would be able to trust the reliability of the documentation when reviewing patients' records.
Using automated safety features and a broad range of patient data, EHR systems allow for becoming much less prone to preventable medical errors, and assist in making clinical decisions more safely.
Electronic Health Record systems not only enhance the operational performance of healthcare organizations but also improve clinical decision-making within them. The administrative processes which once needed to be documented manually in large amounts can now be handled digitally, thereby grouping less work on the hands of the healthcare personnel and enhancing the overall performance in work.
EHR systems combine various administrative and clinical procedures in a system. All of this could be done within the same digital space, which includes appointment scheduling, clinical documentation, prescription management, and billing. The integration has the benefit of eliminating the necessity of a separate software system, and also many of the manual functions of traditional healthcare record management.
EHR systems have digital documentation tools that enable clinicians to document patient encounters more effectively. The features include structured templates, voice recognition, and automated data entry, enabling physicians to record clinical notes with minimal time spent on administrative processes. This will enable the healthcare providers to spend more time attending to the patients.
The benefits of operational efficiency are also applied to management in hospitals and administration. EHR systems produce data that healthcare organizations analyze to track workflow bottlenecks, patient throughput, and resource utilization. Such insights can help administrators to maximize the staffing level, minimize waiting time, and enhance service delivery.
Also, built-in billing and coding can help health care organizations simplify revenue cycle operations. EHR systems decrease medical coding errors and enhance the quality of insurance claims made by connecting clinical documentation to billing procedures.
Through these operational enhancements, EHR systems enable healthcare organizations to become increasingly efficient in providing care while maintaining high clinical quality standards.
Although traditional healthcare systems were once concerned with treating illness only after symptoms appeared, new healthcare trends increasingly emphasize prevention and health maintenance. Electronic Health Record systems are also very important to facilitate this transition by offering healthcare organizations access to vast amounts of patient-related information that could be structured and analyzed to reveal health risks and demographic trends.
Healthcare providers can use EHR platforms to monitor health indicators of patients over time, including vital signs, laboratory results, chronic disease markers, and treatment outcomes. Using this data, clinicians can detect the warning signs of disease progression at an early stage and act before the condition deteriorates.
These capabilities are very useful in preventive care programs. The EHP systems allow the automatic generation of alerts when it comes to regular screenings, inoculations, and follow-ups basing on the demographics and medical history of the patient. Such automatic reminders are used to make sure that patients are provided with the necessary preventive care services within the correct timeframes.
EHR systems also play a critical role in population health management initiatives since data collected by the EHR systems can be used. Health organizations can use aggregated patient data to determine trends in terms of the prevalence of chronic diseases, the effectiveness of treatment, and the use of health services. These lessons can help healthcare professionals to develop specific public health interventions and disease management programs.
Constant follow-up and coordinated attention are requirements for patients with chronic illnesses like diabetes, heart ailments, and breathing problems. EHR systems facilitate these programs by delivering complete information to clinicians on the progress and adherence to treatment and clinical outcomes of patients.
With EHR systems facilitating the creation of data-driven healthcare strategies, it is possible to transform the current healthcare organizations by not responding to illnesses but providing preventive and proactive care models. This change eventually results in better patient outcomes, and more sustainable healthcare systems.
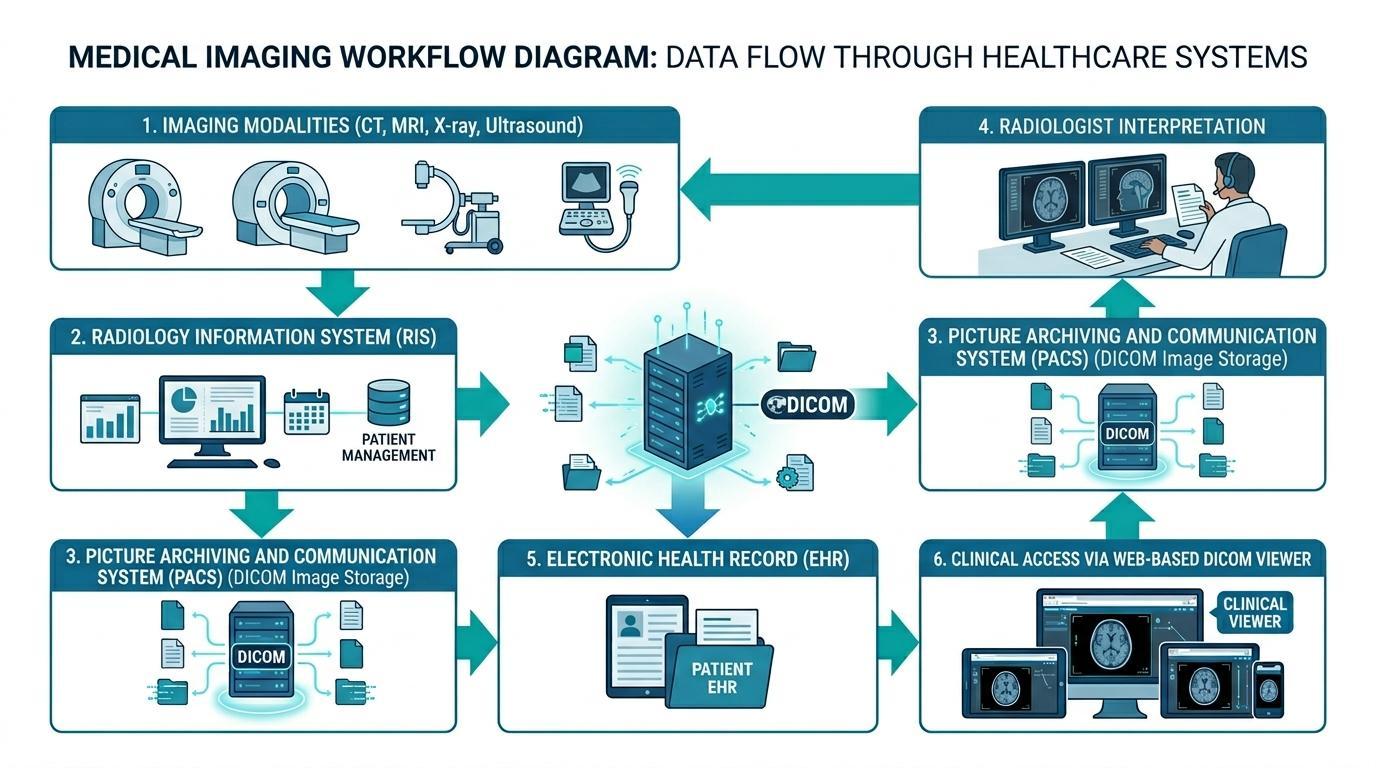
Electronic Health Record and then into a web-based DICOM viewer, helping clinicians to access the study. Above is a diagram of how do PACS integrate with RIS and EHR Systems.
Diagnostic imaging is very important in healthcare decision-making today. X-rays, CT scans, MRI, and ultrasounds are imaging technologies that provide clinicians with the information needed to properly diagnose and develop treatment plans. Nonetheless, the usefulness of these imaging studies is strongly influenced by how easily they can be accessed and interpreted by clinicians within the overall clinical workflow.
Electronic Health Records are systems connected to the medical imaging infrastructure to ensure that diagnostic imaging data is accessible alongside other patient health data. This integration is usually achieved by connecting EHR platforms to imaging technology, such as Radiology Information Systems (RIS) and Picture Archiving and Communication Systems (PACS).
PACS systems are responsible for storing, managing, and distributing medical imaging data in standardized formats such as DICOM. These systems enable radiologists to view imaging studies, make diagnostic findings, and write radiology reports. After conducting the imaging analysis, the appropriate reports and image references may be integrated into the patient's EHR record.
If EHR systems are connected to PACS platforms, clinicians might be able to view imaging findings in the patient's electronic chart. For example, a doctor accessing a patient's records in the EHR system can view diagnostic images through an embedded web-based DICOM viewer without leaving the clinical interface. This is a smooth flow of workflow without the necessity to log into different systems of imaging, and the efficiency of clinical decision-making is greatly enhanced.
EHR systems and imaging platforms integration also improves the interaction between radiologists and referring physicians. Once the imaging outcomes are connected with the digital record of the patient, the clinicians in various departments can access the same diagnostic data and do it simultaneously. The ability facilitates the discussion of cases across different disciplines, treatment planning sessions, and teleconferences with specialists based in other medical institutions.
With healthcare entities expanding their usage of digital imaging technologies, the migration of EHR systems to integrate with cloud PACS imaging system will be of more significance. Such associations allow caregivers to integrate clinical records and diagnostic imaging data to form a more detailed and comprehensive picture of a patient's health. That’s how Cloud-Based PACS is revolutionizing Telemedicine.
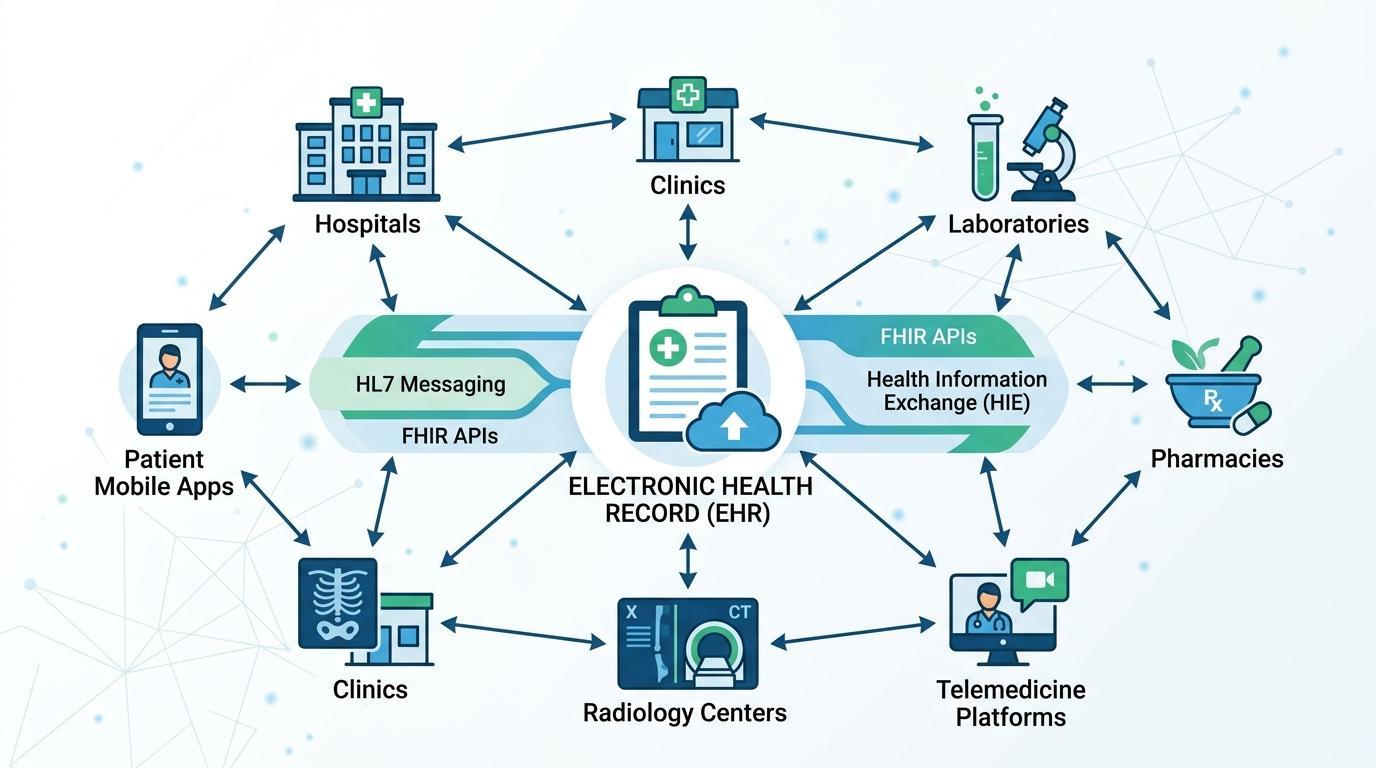
One of the most significant features of the modern Electronic Health Record systems is called interoperability. The capacity to share patient information between various systems, organizations, and even regions is becoming a strong demand by healthcare organizations. In the absence of interoperability, essential patient data may be divided between independent platforms and cursory arranged care.
To overcome this dilemma, healthcare technology standards have been developed to facilitate orderly communication among various healthcare systems. Health Level Seven (HL7) is one of the most popular messaging frameworks that permits healthcare applications to communicate clinical data, including patient admissions, laboratory results, and medication orders.
More still, the Fast Healthcare Interoperability Resources (FHIR) standard has become a current model of healthcare data sharing. FHIR is based on a web-based API to allow healthcare applications to share structured patient information in real time in a secure manner. This practice enables EHR systems to integrate more effectively with third-party applications, patient portals, mobile health systems, and research databases.
EHR systems can be used to communicate with a great variety of healthcare technologies through interoperability frameworks like HL7 and FHIR. These include laboratory, pharmacy, imaging, insurance, and telemedicine systems. The outcome is a health IT ecosystem that is more connected and has data flows that are seamlessly flow between the systems that assist in diagnosis, treatment, and care management.
The interoperability is also critical for cross-institution collaboration. There are usually many healthcare providers that treat patients, such as hospitals, specialist clinics, and community healthcare centers. EHRs with interoperability across these providers enable the sharing of patient records, eliminate test duplication, and support continuity of care.
With the ongoing development of digital healthcare infrastructure, interoperability will be a focus of healthcare technology development. Newer connected healthcare applications can now communicate effectively, safely, and fast with their counterparts due to standards like FHIR.
EHR systems are continually expanding with new technologies that healthcare organizations implement to improve patient outcomes and operational efficiency. New developments are emerging that broaden the scope of EHR platforms beyond record management to include intelligent systems that actively facilitate clinical decision-making.
The integration of artificial intelligence and machine learning technologies into EHR systems can be considered one of the most promising approaches in this direction. Clinical decision support tools based on AI can process large amounts of patient data, identify trends, flag potential health risks, and suggest evidence-based treatment plans. The capabilities enable clinicians to make better decisions and minimize the cognitive burden of complicated patient cases.
Another domain that is showing tremendous value by EHR platforms is predictive analytics. With the help of historical patient data analysis, healthcare organizations can determine trends in regards to disease development, risk of readmission, and treatment efficacy. Such insights can guide health providers to act sooner and plan prevention care strategies that would yield better patient outcomes in the long term.
EHR platforms are as well getting more integrated with patient engagement technologies. Protective patient portals, mobile health, and remote monitoring systems allow patients to manage their health records, contact healthcare professionals, and monitor individual health statistics. Such a high degree of transparency stimulates patients to be more active in their health management.
EHR systems are also changing the methods of implementation and administration with the use of cloud computing technologies. Healthcare infrastructure in the cloud enables healthcare organizations to scale their systems more effectively, allows clinicians to access them remotely, and helps them adopt new healthcare technologies faster. The flexibility is especially useful in a world where telemedicine and distributed models of healthcare delivery are gaining momentum.
EHR platforms will implement digital healthcare ecosystems as healthcare systems continue to embrace a modernized approach. The fact that they can merge data, aid in clinical decision-making, and facilitate collaboration across healthcare networks will be key in determining the future of patient care.
Electronic Health Records systems have radically changed how health care organizations handle patient data and provide clinical care. EHR systems help healthcare professionals retrieve full patient information safely and quickly by replacing disjointed paper documents with centrally located digital platforms.
The effects of these systems are evident across many areas of healthcare provision. Clinical decision-making improves, collaboration between care teams is supported by better communication tools, and medical errors decrease with automated safety measures. Simultaneously, unified workflows and analytics can help healthcare organizations work more effectively and plan proactive health management.
Interoperability is also essential for integrating EHR systems with other healthcare technologies. Patient information may be exchanged between institutions and connected to imaging platforms, laboratory systems, and telemedicine services through a standardized structure, including HL7 and FHIR. Such relationships establish an integrated healthcare ecosystem in which clinicians can work in coordination and patients receive coordinated care.
With the ongoing development of digital health technologies, EHR systems will remain a focus of healthcare innovation. By enabling safe data sharing, supporting sophisticated analytics, and introducing new technologies, including artificial intelligence, EHR platforms will continue to enhance the quality, efficiency, and accessibility of patient care.
Electronic Health Record system is an online system where patient health records are managed and kept in a central database. EHR Systems enable healthcare providers to retrieve patient records, clinical notes, lab results, imaging reports, medications, and treatment histories in real time, which enhances healthcare delivery coordination and effectiveness.
Patient safety is enhanced with the EHR system since it has built-in automated features, like medication interaction alert systems, allergy alerts, and clinical reminders. These characteristics can assist medical workers in determining the possible risks prior to treatment provision, minimizing the possibility of avoidable health care mistakes.
The EHR systems include medical imaging systems like PACS and RIS. The integration will enable clinicians to view diagnostic imaging and radiology reports directly in the patient's electronic record. Integrated DICOM viewers in most instances allow a physician to access imaging studies without being taken out of the EHR interface.
Interoperability refers to the ability of different healthcare systems to exchange and interpret patient data. Standards such as HL7 messaging protocols and FHIR APIs enable EHR systems to communicate with laboratory systems, imaging platforms, pharmacy databases, and other healthcare technologies.
EHR systems support preventive healthcare by enabling clinicians to track patient health indicators over time and identify potential risk factors. Automated reminders for vaccinations, screenings, and follow-up visits help healthcare providers implement preventive care strategies that improve long-term patient outcomes.
|
Cloud PACS and Online DICOM ViewerUpload DICOM images and clinical documents to PostDICOM servers. Store, view, collaborate, and share your medical imaging files. |